Infectious Disease
The autonomy of patients to issue a non-resuscitation prescription in the event of a COVID-19 hospitalization
Source / information
Published by:
Source:
J. Kirupakaran et al. Early career research. Presented at: American Society for Preventive Cardiology Congress for the Prevention of Cardiovascular Disease; 23-25 July 2021 (virtual meeting).
Disclosure:
Kirupakaran does not report any relevant financial information.
ADD SUBJECT TO EMAIL ALERTS
Receive an email when new articles are published on
Please enter your email address to receive an email when new articles are published on . “data-action =” subscribe “> subscribe
We could not process your request. Please try again later. If this problem persists, please contact [email protected].
Back to Healio
For high-risk patients, a discussion about ordering non-resuscitation should take place before hospitalization, as only 10% of patients had the autonomy to do so after admission due to severe COVID-19, a spokesman reported.
“CPR, as originally designed, was reserved for cardiac arrest patients who were in good health prior to the event. It has since become the standard of care for all patients in cardiac arrest, “said Johnathan Kirupakaran, DO, senior resident in the medical division of Woodhull Medical Center in Brooklyn, New York, during a presentation to the American Society for Preventive Cardiology Congress on CVD -Prevention. “However, hospital CPR survival rates remain very low. Rates are estimated to be less than 20% and survival to discharge near 0%. Variables that can affect CPR survival … especially age, race, sepsis, and pneumonia are significant in the context of COVID-19. [In two publications], the survival rate from hospital cardiac arrest in patients with COVID-19 was less than 11%. “

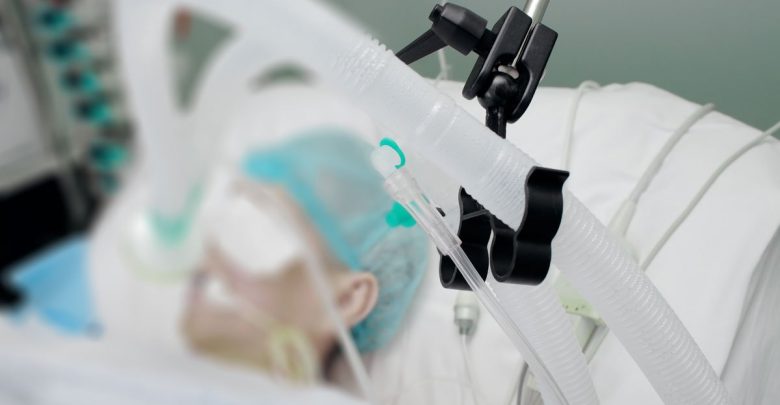
Source: Adobe Stock
Researchers at Woodhull Medical and Mental Health Center evaluated demographic, clinical and outcome data on 520 people admitted between March 20 and May 5, 2020 for COVID-19. Of these patients, 115 had documented no-resuscitation orders (DNR). Interesting findings included survival to discharge, DNR ordering within 24 hours of admission, and the identity of the DNR decision maker.
Of the patients with DNR prescriptions hospitalized for COVID-19, approximately 53% were men, 53% were Hispanic American, and the mean age was 77 years.
In comparison, those without a DNR order were predominantly men (61%) with a median age of 59 years. As in the DNR group, most of these patients were Hispanic American (53%).
The researchers found that 29.6% of patients with DNR prescriptions were placed prior to COVID-19 hospitalization or within 24 hours of admission.
Kirupakaran and colleagues also observed that 3.5% of DNR orders were placed relatively late in the patient’s clinical course, following cardiac arrest with CPR performed and spontaneous circulation returning.
Overall, 10.4% of patients placed their own DNR orders directly, while 83.5% of orders were placed by a surrogate mother or a health care representative.
Placing DNR orders in patients admitted to hospital with COVID-19 was associated with a higher risk of hospital mortality compared to the non-DNR group (OR = 17.346; 95% CI, 9.9805-30.145 ; P <0.001).
In addition, 15.7% of patients with DNR prescriptions survived to discharge.
“CPR is an invasive, traumatic cardiovascular intervention. Ethical considerations about CPR are important, especially with an aging American population, ”said Kirupakaran. “Adequate patient education just before a critical event occurs is critical to maintaining patient autonomy and ensuring that they make the decision for themselves. The training on CPR outcomes offered by health care professionals remains largely diverse; however, the use of decision aids such as the pre-arrest morbidity score can be used to explain the results.
“More research is needed on the impact of educational status and religious background on CPR education,” said Kirupakaran. “The other important aspect of this project is considering ethics as an important aspect of preventive cardiology. While you are working to prevent disease onset or worsening, it is also important to prevent undue harm from the treatments we offer. “
The presentation won third place in the Early Career Presentations competition.
References:
ADD SUBJECT TO EMAIL ALERTS
Receive an email when new articles are published on
Please enter your email address to receive an email when new articles are published on . “data-action =” subscribe “> subscribe
We could not process your request. Please try again later. If this problem persists, please contact [email protected].
Back to Healio







